 I received a surprising amount of hits from my recent shoulder surgery updates and also received a bunch of questions from viewers, as well as, those of you who are considering surgery yourself. So I figured now that I’m well enough to type this would be a good time to catch you up on where I stand today two full weeks after my surgery.
I received a surprising amount of hits from my recent shoulder surgery updates and also received a bunch of questions from viewers, as well as, those of you who are considering surgery yourself. So I figured now that I’m well enough to type this would be a good time to catch you up on where I stand today two full weeks after my surgery.
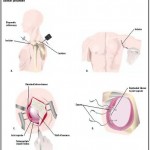
Two weeks ago (10/21/09) I underwent Open Bankart Shoulder Surgery (info here) to fix continuous dislocations of my right shoulder. I had a large group of muscles in the front part of my shoulder torn (see older article here on that). I had to undergo an initial X-Ray to confirm the dislocation was occurring and then a closed MRI to confirm what muscle groups were torn. Once that was determined they did a follow up physical and scheduled surgery.
The whole process (from final severe dislocation to surgery) took about a month to go through.
Surgery itself is described as walk in and walk out. That is if all is well and there are no complications. In my case, the muscle damage was far more severe than they thought. The doctor could only determine this once he had me fully opened. My doctor feared there was more damage than the MRI showed and that’s why he went with the open verses Laparoscopic, which has much smaller incisions then the open. The risk with Laparoscopic is the surgeon may not see the full extent of damage. Laparoscopic and open incision both have the same healing time requirement (12 weeks) though I’ve been told the initial pain from Laparoscopic is much less than open incision as there is less cutting. Open incision has the higher success rate according to my orthopedic surgeon and again– also is the most painful surgery to recover from.
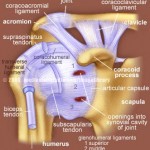 Surgery preparation was less than an hour. The night before I had to shower completely, dry off completely, and then apply an antiseptic scrub to my entire arm and right torso (scrubbing the body for 10 minutes). The next morning I had to scrub for 10 more minutes and put on a new shirt (button up style so it’s easier to get on/off). I could not eat or drink after midnight of the proceeding night to my surgery. I also could not take my stomach acid medicine. When you get to the hospital you strip down to your underwear and put on a medical gown. I was dropped off by my wife around 10 am and actual prep started at about 11 am. They then have you meet with the post-op nurse, the operation room nurse, the anesthesiologist, and finally the doctor. You fill out allergy paper work, sign over consent to operate to the doctors, and also consent to being sedated. You also confirm what body part you’re having operated on and what type of surgery (they do this some five time orally and two times in written sign off). The doctor marks your arm with a marker. Again, this all takes about an hour.
Surgery preparation was less than an hour. The night before I had to shower completely, dry off completely, and then apply an antiseptic scrub to my entire arm and right torso (scrubbing the body for 10 minutes). The next morning I had to scrub for 10 more minutes and put on a new shirt (button up style so it’s easier to get on/off). I could not eat or drink after midnight of the proceeding night to my surgery. I also could not take my stomach acid medicine. When you get to the hospital you strip down to your underwear and put on a medical gown. I was dropped off by my wife around 10 am and actual prep started at about 11 am. They then have you meet with the post-op nurse, the operation room nurse, the anesthesiologist, and finally the doctor. You fill out allergy paper work, sign over consent to operate to the doctors, and also consent to being sedated. You also confirm what body part you’re having operated on and what type of surgery (they do this some five time orally and two times in written sign off). The doctor marks your arm with a marker. Again, this all takes about an hour.
You are then given an IV so they can administer liquids direct to your circulatory system. I had the IV put in my left hand in the vein on the top of your hand. There’s a severe pinch and it will be sore for at least 24 hours. You have to just deal with it. You lay down for 10 minutes and get comfortable on a cot.
You’re wheeled on a cot into pre-operation where they begin with liquid anesthesia. You are then given (if you agreed to do so during the questioning earlier) a nerve block by the anesthesiologist. This is four needle shots into four different nerve endings in your neck. Each shot you tell the anesthesiologist what part of your arm is numb. After all four shots you whole arm goes numb within five to ten minutes. Once they are sure your numb (you’re still somewhat awake and can tell them) they roll you into the operating room. You’re covered with blankets and a tube is put under them that blows hot air. The operating room is very cold to keep germs down (as is most of the hospital). Once they are sure you’re both warm and comfortable the surgeon ask you if you’re ready to begin. Once you say yes they give you the final liquid anesthetic. They hook up all the heart and breathing monitoring tabs on your body. Within one minute you’re asleep.
Once you’re asleep they put a tube in your throat via your mouth to administer oxygen. They then being the procedure.
You wake up in recovery, which is near pre-op staging. Your arm is in a sling and entirely numb. You have oxygen being given through your nose. Your throat is sore from the previous throat administered oxygen though the tube is long gone. The sore throat will last about two days and is minor in nature.
I was supposed to be under for two hours tops, but because they found so much damage I was under for almost four hours. You’re still covered by blankets and on the IV. The anesthesiologist checks on you first and asks you to move your fingers. He then tells you to take deep consistent breaths to “blow off” the anesthetic. For whatever reason there was only one nurse in recovery. For reasons still confusing to me she throws a fit that there are two patients in there and says she cannot watch us both. They send for my operating room nurse who then moves me into pre-op. She sits with me for the next twenty minutes while I come to.
The orthopedist then visits with me to tell me about the extent of the damage and that all went well. He tells me my blood pressure is a bit high (170/90) and that when I get fully awake they’ll give me pain killers to take it down. He states it’s from the extended length of sedation. They then wheeled me back into the first room I was in when this all started (the general recovery area). I sit there another twenty minutes and slowly come to. I can feel the heavy amount of pain in my arm despite the nerve block. Because of the nerve block I cannot move my right side. They then called my wife and let her know she could come to see me, as well as, maybe bring me home.
Twenty more minutes go by and it’s nearly 6 pm when my wife arrives. I tried to stand up, but I’m still too weak from being under so long. Because I was still in pain, they give me a percocet pain killer. This makes me instantly nauseous. By 6:30pm I’m able to stand long enough to use the bathroom and urinate. At this point my blood pressure is down to 140/85. Still not normal, I’m still dizzy, still in pain, and still cannot stand. The post-op nurse decides to admit me for over night monitoring.
They wheel me up stairs in a wheel chair and move me into their orthopedic recovery wing, which I’ll later find out is self care. How partially crippled people end up in self care is beyond me, but fortunately the nurses do help out a lot more than they probably are supposed to.
The hospital would rather you did not stay over night for two reasons. First, because keeping me there under 24/7 monitoring is mighty expensive. Second, because the longer I’m there the more risk there is I’ll catch something as the nurses move between the orthopedic recovery wing to the general population recovery area (where the swine flu sufferers hang out amongst others), which shares the same floor as my room and is the next hall over.
They sit me in an upright position in the hospital bed and immediately I feel better. The hospital bed is much wider and had a better mattress than the same day surgery cots. The room is slightly warmer as well. I’m on the same IV bag from downstairs and they hook me up to a blood pressure machine. I’m sharing the room with one other patient and it is the smallest room in the hospital for two of the largest guys they arguably have there. My roommate, Nick, is 49 years old and in for complete right knee replacement. It’s around 7 pm so I missed dinner. They bring me a small cup of chicken broth and crackers. I get another percocet and am told they’ll give me another one in four to six hours.
Nick and I decide to watch ESPN. We each have our own flat screen TV with a limited DirecTV line up, but there is no way in a room barely big enough for our two beds we could have both going at once. Fortunately we’re both into sports and stick with that theme for the night.
Around 10 pm my blood pressure comes down to 130/75 and they take me off the machine. The liquid anesthesia has worn off, but the nerve block will last until around 4 pm the next day. I fall asleep around 11 pm. I’ll be woken up every six hours from there in by a nurse who will take my temperature, my blood pressure, check my IV, and give me pain medicine. This goes on 24/7 whether you’re sleeping or awake. The bath room is shared between two rooms and has no shower. You cannot get up anyway.
The next morning is horrible. As you approach 24 hours from the beginning of surgery the pain starts to come through. They up your pain meds at that point. I can get up with a lot effort and walk. My blood pressure is finally down to 120/70 and my doctor/orthopedist stops in. He checks me over. The anesthesiologist also stops in. I let him know as each finger starts feeling again I get spasms in my arm. He lets me know that’s normal.
By the time my wife is allowed to take me home the nerve block has worn off. They put me on two 5mg Oxycodin with 325mg of Acetaminophen (I’m told this is Vicodin but who knows) every six hours. I’m told to keep my arm in the sling 24/7 and am allowed to only move my hand and lower arm. I’m also told I can sponge bathe, but cannot get the bandages under the sling wet. While bathing I can have the sling off, but must support my arm with my other good arm.
I don’t think about bathing at that point. I basically lay in bed from the time I get home Thursday (10/22) night to Saturday morning (10/24). I get up only to urinate. The first 72 hours are complete Hell pain wise. Every day gets better from there.
I start on 10/24 being able to wash my face and brush my teeth. The next day (Sunday- 10/25) my wife is able to have me stand long enough so she can wash my hair. I then sponge bathe quickly with baby wipes. This is about as far as I move for the first week. Just shy of a week (Tuesday 10/27) I’m finally able to walk around in minor discomfort. My wife is then able to help me through my first sponge bath. I’m also able to finally walk downstairs to eat so I don’t have to sit in bed completely all day. Since coming home I have not worn a shirt. I cannot get it on without being in severe pain. My lounging around shirtless becomes as common as most of the guys you see being chased in “Cops” on TV. I finally am able to pass stool on 10/28. Apparently the Vicodin constipates you for a bit.
On 10/29 my appetite finally comes back. I’d mostly been eating light meals until that point. I’m able to walk around on Halloween (10/31) for trick or treating for about an hour and half. After that I’m exhausted and back in pain again. I also manage to wear a shirt for about three hours while I’m out and at my Mother’s with the family.
On 11/1 (just two weeks shy into recovery) my meds are reduced to one Vicodin every six hours. I can sponge bathe myself at this point except for washing my hair. 11/3 I have my first post-op follow up with my orthopedist. He takes off my bandages and tests my arm. Everything is intact and I have no infection in the wound. They stitched me back up with clear self dissolving stitches so they don’t have to pull anything out of me. They do have to cut each end off of the stitch though that was left for slack and to keep it secure while I healed. The stitches then pull into your skin and will dissolve on their own from there. During the check up I pass out briefly while they test the limits of my range of motion. I’m told this fairly normal. I’m out for no more than 10 seconds. They lay me down, put cold towels on my neck and forehead, and raise my legs. I come to and am back to normal in 10 minutes.
When I get home I’m allowed to take my first full shower. I do so happily. I also only need to wear the sling at night. I’m given an exercise I must do three times a day (you basically use your body to move your arm while it hangs at your side) and am told my only limitation is I cannot raise my bicep any higher than my collar bone line. I’m also given a prescription for physical therapy and told to along with the Vicodin take two tablets of Ibuprofen three times a day.
Since then I’ve been doing my exercises. I’ve also been told to type to spur blood flow in my right arm (a great excuse to make this blog). I can finally also wear a tee shirt. Tomorrow I’m going to call a physical therapist who is nearby. I’m hoping to either line them or another local PT who accepts my insurance provider for payment so I can get my therapy going. I’ll have to go there twice a week for the next twelve weeks.
I hope this answers a lot of your questions and gives you some insight into the recovery process. I’m about 35% back to normal as far as my arm goes. I’m told within six weeks I’ll be at 50% with PT. I’ll be sure to post any milestones as I go through the process so you can see how this whole shebang progresses.
I have not been at work since the day of surgery. It hurts to stand or do any sustained activity for more than an hour or so. That makes work tough, as well as, a lot of other things. Therefore sick time is a must if you plan on getting shoulder surgery and you should clear at least six weeks with your employer from the day of your surgery. I did this by saving up my sick time over the last two years and banking as much time as possible knowing eventually I’d need it for shoulder surgery. If possible, apply for FMLA and short term disability to protect your job. Talk with your HR or local government benefits official to find out more about that. You’ll have to do some preliminary paper work and your doctor will also have to do some. There is a few follow up forms and I’m expected to give NY state monthly medical reports on my recovery. I cannot return to work until I get a note from my orthopedist saying I’m cleared to do so. As such, I’ve setup a six week follow up appointment on 11/23 with the intention to get clearance to return the following week. I should be four weeks into PT at that point if all goes well.


Cody, I’m glad to hear you found the site useful. I am now fully recovered. I’ve been weightlifting as prescribed by my Physical Therapist for some two weeks now. I’m seeing minor discomfort in my tendons, but overall my strength is 100% of what it was pre-injury. I wish you the best of luck and my only advice is to stick with the PT and to be sure to have open conversations with your medical professionals. This will insure quick and complete recovery. Thank you again for stopping in and letting me know what you think about the site. It is appreciated.
I am two weeks plus one day post-op. I had a right shoulder arthroscopy due to a hill sacs lesion from multiple dislocations over the past four years. My pain with no movement is very minimal, however sometimes during my at home therapy movements can have a sharp pain. I am still wearing a sling and using only my left hand. I have yet to have any complications and start PT next week. I’m very excited to get through PT and start playing sports again. I just found your blog tonight and it has been very useful.